
In the journey toward parenthood, the focus is frequently placed on the woman, yet clinical data shows that male factor infertility is a contributing factor in nearly 50% of all infertility cases. Unlike many health conditions, male reproductive challenges often remain "silent" because they rarely present physical symptoms that affect daily life. These issues typically stem from problems with sperm production, sperm transport, or functional difficulties. Just as certain conditions affect women—which you can explore in our guide on female factors of infertility—men also face biological and environmental hurdles that can impede conception. Recognizing red flags like testicular pain, changes in sexual function, or abnormal semen analysis is the first step toward effective treatment.
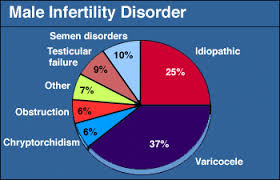
A varicocele is an enlargement of the veins within the loose bag of skin that holds your testicles (scrotum). This is the most common reversible cause of male factor infertility. It causes abnormal temperature regulation around the testes, which significantly impairs sperm motility and morphology.
Infections can interfere with sperm production or health, or can cause scarring that blocks the passage of sperm. These include inflammation of the epididymis (epididymitis) or testicles (orchitis) and certain sexually transmitted infections (STIs) like gonorrhea or HIV.
Retrograde ejaculation occurs when semen enters the bladder during orgasm instead of emerging out through the penis. Various health conditions can cause this, including diabetes, spinal injuries, and medications. This often leads to azoospermia, where no sperm is found in the semen despite normal production.
Cancers and nonmalignant tumors can affect the male reproductive organs directly or affect the glands that release hormones related to reproduction, such as the pituitary gland. Furthermore, the radiation or chemotherapy used to treat tumors can severely impact male fertility.
Sperm are carried through various tubes. Blockages can occur due to various reasons, including inadvertent injury from surgery, prior infections, trauma, or abnormal development, such as in cystic fibrosis. This results in obstructive azoospermia, where sperm is produced but cannot be ejaculated.
These include trouble achieving or maintaining an erection (erectile dysfunction), premature ejaculation, painful intercourse, or anatomical abnormalities such as hypospadias (where the urethral opening is on the underside of the penis).
Testosterone replacement therapy, long-term anabolic steroid use, certain antifungal medications, and some ulcer drugs can impair sperm production and decrease male fertility by disrupting the delicate hormonal balance.
Certain surgeries may prevent you from having sperm in your ejaculate. These include vasectomies, inguinal hernia repairs, scrotal or testicular surgeries, prostate surgeries, and large abdominal surgeries performed for testicular and rectal cancers.
Elevated temperatures in the scrotum impair sperm production. Frequent use of saunas or hot tubs can temporarily lower sperm counts. Similarly, sitting for long periods, wearing tight clothing, or working with a laptop directly on your lap may increase scrotal temperature and impact fertility.
Drinking alcohol can lower testosterone levels and cause erectile dysfunction. Tobacco use (smoking) is well-documented to decrease sperm count and motility while increasing sperm DNA fragmentation.
Severe or prolonged emotional stress can interfere with the hormones needed to produce sperm. Depression may also lead to sexual dysfunction, creating a stressful cycle that further complicates the path to conception.
If you have concerns regarding male reproductive health or need a detailed semen analysis, our experts are here to help.
© Copyright 2021 Dr. Parzan Mistry.
Designed and Developed by EDM